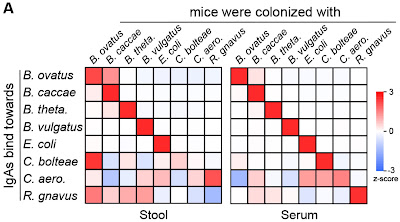
Mitochondria make ATP through oxidative phosphorylation, thus providing energy for nearly all cellular functions. Many human disorders are attributed to mitochondrial dysfunction. Their functions seem narrow and their genomes, known for decades, were reduced to encoding a mere 13 proteins after transferring most to the nuclear genome. However, these authors note that ‘hundreds of mitochondrial proteins lack clear functions’. They previously (Stefely 2016) applied mass spectroscopy (MS) ‘multiomics’ to assign functions to mitochondrial uncharacterized (x) proteins (MXPs) in yeast. Here, they generated using CRISPR over 200 knockout (KO) cell lines, targeting 50 nuclear genes encoded MXPs plus 66 with known functions, and assessed in each line over 8,000 proteins, over 3,000 lipids and over 200 metabolites by MS (epic undertaking!). They found high reproducibility and dynamic range, with ‘many molecules showing regulation over 3-4 orders of magnitude’.
Some assessments confirmed expectations or were mild surprises, e.g.,
the importance of ALDH18A1 or NADK1 in proline synthesis (Fig 2a).
Others revealed ‘new biology’, such as a key role for the putative zinc
transporter SLC30A9 in mitochondrial ribosome and OxPhos proteins (Fig
2e, shown). They also found that one ’upstream (open) reading frame’
(PYURF) is a chaperone essential for complex I and coQ
synthesis, linked a transporter (SLC30A9) to ribosomes, and found a
second gene (RAB5IF) contributing to developmental
disorders. They offer their “8.3 million distinct
biomolecule measurements” online to help others ascribe additional
functions, a promising resource.
NB PubPeer comment raises concerns regarding the methods, interpretations, and conclusions.